Reports
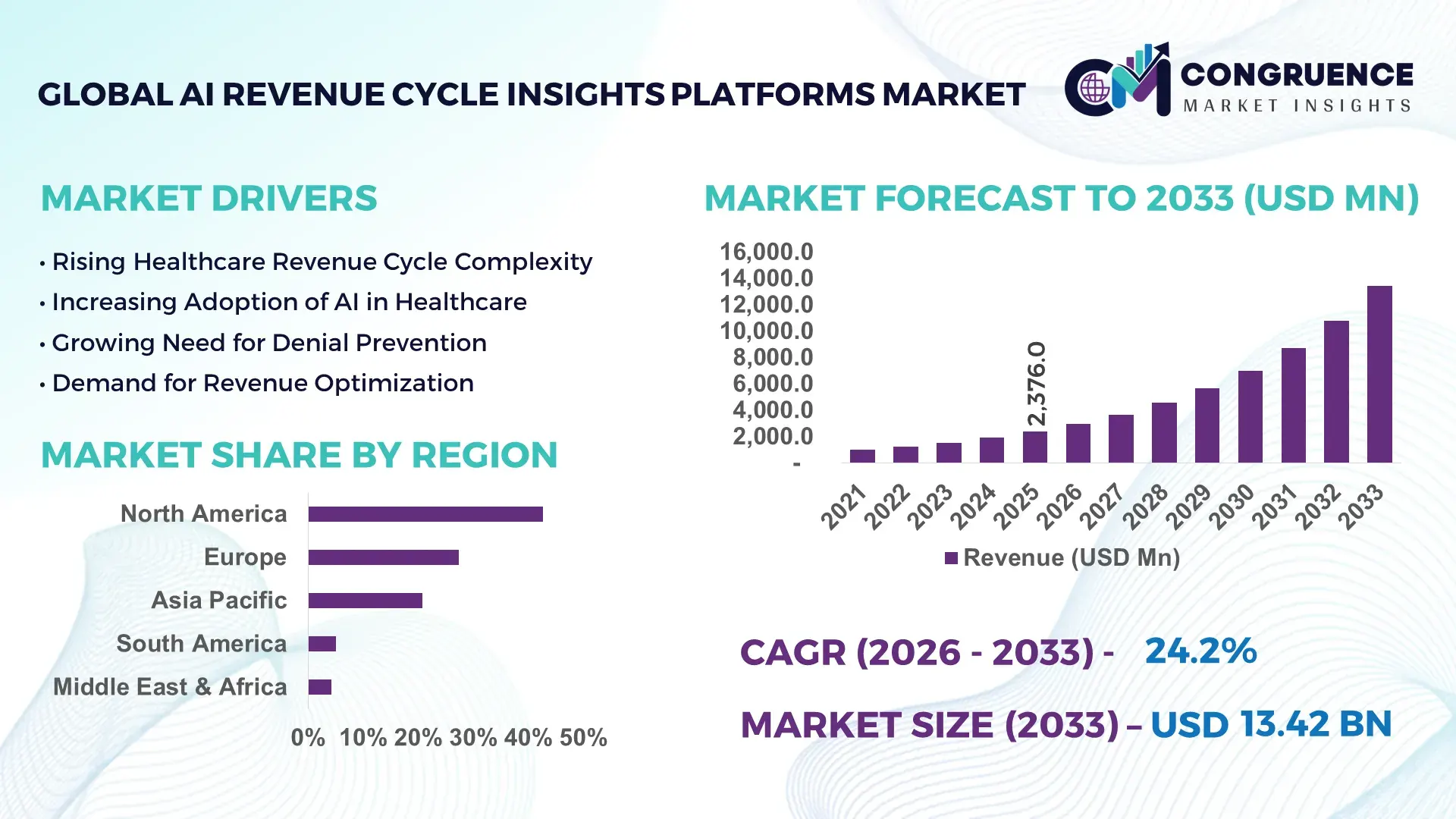
The Global AI Revenue Cycle Insights Platforms Market was valued at USD 2,376.0 Million in 2025 and is anticipated to reach a value of USD 13,418.4 Million by 2033 expanding at a CAGR of 24.16% between 2026 and 2033, according to an analysis by Congruence Market Insights. The growth is primarily driven by increasing healthcare data volumes and the need for automated analytics to optimize claims management, billing accuracy, and reimbursement cycles.
The United States remains the most technologically advanced environment for AI revenue cycle analytics deployment, supported by one of the world’s largest healthcare IT ecosystems. Over 5,200 hospitals and more than 200,000 physician practices in the U.S. actively deploy digital revenue cycle systems integrated with predictive analytics. Healthcare IT spending in the country surpassed USD 230 billion annually, with AI-based financial analytics tools gaining rapid adoption among multi-hospital networks and payer-provider partnerships. Approximately 62% of large hospital systems have integrated AI-based claim denial prediction tools to automate revenue monitoring, while over 48% of healthcare providers use predictive analytics dashboards to track payer behavior and reimbursement patterns. The U.S. also hosts a large concentration of healthcare AI startups—over 450 firms focused on healthcare finance analytics, many supported by venture funding exceeding USD 6 billion in the past five years.
Market Size & Growth: The market was valued at USD 2,376.0 Million in 2025 and is projected to reach USD 13,418.4 Million by 2033, expanding at 24.16% CAGR, driven by the growing need for predictive analytics in healthcare billing and reimbursement optimization.
Top Growth Drivers: Approximately 65% of healthcare providers are adopting automated claims analytics; AI reduces claim denial rates by nearly 35%, while predictive billing insights improve collection efficiency by 28%.
Short-Term Forecast: By 2028, AI-driven revenue analytics platforms are expected to improve healthcare billing accuracy by 32% and reduce operational costs in revenue cycle departments by 25%.
Emerging Technologies: Adoption of predictive denial management, natural language processing for coding automation, and machine learning-based reimbursement forecasting is accelerating across healthcare financial systems.
Regional Leaders: North America is projected to exceed USD 6.2 Billion by 2033 due to large hospital networks; Europe may approach USD 3.4 Billion with strong digital health infrastructure; Asia-Pacific could reach USD 2.6 Billion driven by hospital digitization programs.
Consumer/End-User Trends: Large hospital groups and multi-specialty clinics represent more than 58% of deployments, while payer organizations increasingly integrate AI analytics to optimize claim approval cycles.
Pilot or Case Example: In 2024, a U.S. healthcare network implemented AI-driven denial prediction tools, improving reimbursement turnaround times by 29% and reducing manual claim reviews by 41%.
Competitive Landscape: The market leader holds roughly 18% share, followed by major players such as Oracle Health, Optum, Change Healthcare, Experian Health, and Waystar, competing through advanced analytics platforms.
Regulatory & ESG Impact: Healthcare organizations are aligning AI revenue cycle tools with compliance frameworks such as HIPAA and healthcare price transparency regulations, encouraging secure data management and billing transparency.
Investment & Funding Patterns: Global venture capital investments in healthcare financial AI solutions surpassed USD 4.5 Billion between 2022–2025, supporting startups focused on predictive claims analytics and automation.
Innovation & Future Outlook: Integration with cloud-based healthcare data platforms, generative AI coding assistants, and interoperable health information exchanges is expected to transform revenue optimization workflows.
AI revenue cycle insights platforms are increasingly integrated across healthcare payer-provider ecosystems, with hospitals accounting for roughly 55% of platform adoption, followed by physician groups at 28% and payer organizations at 17%. Innovations in predictive denial analytics, autonomous coding systems, and real-time reimbursement dashboards are accelerating deployment. Strong regulatory push for billing transparency and expanding healthcare digitization in North America and Asia are shaping consumption patterns while advancing AI-enabled financial optimization across healthcare systems.
The AI Revenue Cycle Insights Platforms Market has become strategically critical for healthcare systems seeking to optimize financial performance while navigating increasingly complex reimbursement frameworks. Hospitals and payer organizations process billions of claims annually, and administrative inefficiencies account for nearly 25–30% of healthcare operational costs in several developed economies. AI-driven revenue cycle platforms analyze structured and unstructured data—including billing codes, patient records, and payer policies—to automate denial prediction, payment forecasting, and compliance monitoring.
Modern machine-learning-based claim analytics deliver measurable performance improvements compared with legacy rule-based billing software. For example, predictive denial management algorithms deliver nearly 40% improvement in claim approval accuracy compared to traditional rule-driven systems, significantly reducing manual claim rework. Cloud-based analytics platforms further enable hospitals to process millions of claim transactions daily while generating predictive revenue forecasts in real time.
Regional adoption patterns reveal significant differences in market maturity. North America dominates in deployment volume, supported by large healthcare provider networks and mature electronic health record infrastructure. Meanwhile, Europe leads in AI adoption compliance frameworks, where nearly 52% of healthcare enterprises are integrating AI analytics into revenue management platforms to comply with digital health data regulations and cross-border reimbursement standards.
Short-term market outlook suggests rapid operational improvements as AI capabilities mature. By 2028, predictive coding automation and generative AI billing assistants are expected to improve coding accuracy by nearly 35% while reducing administrative workload by 30%. Healthcare organizations are also aligning AI investments with sustainability and compliance initiatives. Firms are committing to digital workflow optimization that could reduce paper-based billing documentation by over 60% by 2030, contributing to ESG objectives related to operational efficiency and resource reduction.
A practical micro-scenario demonstrates the strategic value of AI adoption. In 2024, a large U.S. hospital network implemented AI-driven claim analytics, enabling automated identification of billing discrepancies and achieving 31% faster reimbursement cycles along with 26% reduction in claim denial rates. Such measurable operational improvements are encouraging broader adoption across healthcare systems worldwide.
As healthcare providers continue digital transformation initiatives, the AI Revenue Cycle Insights Platforms Market is evolving into a foundational technology layer for financial transparency, regulatory compliance, and operational resilience. Its integration with clinical data platforms, cloud infrastructure, and predictive analytics tools positions it as a key pillar supporting sustainable and data-driven healthcare financial management in the coming decade.
The AI Revenue Cycle Insights Platforms Market is expanding as healthcare organizations increasingly rely on advanced analytics to improve revenue management, reduce billing inefficiencies, and enhance payer-provider coordination. Growing volumes of electronic health records, digital billing systems, and insurance claims data are creating a strong demand for automated insights platforms capable of analyzing millions of transactions in real time. AI technologies such as machine learning, natural language processing, and predictive analytics enable healthcare providers to identify claim errors, forecast reimbursements, and optimize billing workflows. Hospitals and multi-specialty clinics are integrating these platforms into enterprise healthcare IT systems to reduce administrative burdens and improve financial transparency. Additionally, digital health infrastructure expansion, payer policy complexity, and rising healthcare costs are intensifying the need for intelligent revenue management tools. Technology vendors are responding by launching cloud-based analytics platforms capable of integrating with hospital information systems, electronic medical records, and insurance databases, creating a more data-driven revenue cycle ecosystem.
Healthcare reimbursement frameworks have become increasingly complex due to evolving insurance policies, payer rules, and regulatory requirements. Hospitals process millions of claims annually, and manual billing systems often struggle to detect coding errors, claim inconsistencies, and reimbursement anomalies. AI-driven revenue cycle insights platforms address this challenge by analyzing historical claim patterns and identifying high-risk claims before submission. Studies indicate that approximately 20–25% of medical claims initially face denial or delay, largely due to coding errors and incomplete documentation. AI analytics systems can automatically evaluate billing records, detect anomalies, and recommend corrective actions before submission. Hospitals implementing predictive denial analytics have reported reductions of nearly 30–40% in claim rejection rates while improving billing workflow efficiency. In addition, automation reduces administrative workload in revenue cycle departments, where staff previously spent several hours manually reviewing claims. The increasing digitization of healthcare records and growing adoption of electronic billing systems across large healthcare networks are further accelerating demand for AI-driven financial insights platforms.
Despite the benefits of advanced analytics, many healthcare organizations face difficulties integrating AI revenue cycle platforms with legacy hospital information systems and fragmented data environments. Healthcare providers typically operate multiple software platforms for patient records, billing management, insurance verification, and clinical documentation. These systems often store data in incompatible formats, limiting seamless integration with AI analytics tools. Surveys of healthcare IT departments suggest that nearly 40% of hospitals still rely on partially digitized or hybrid billing systems, making it difficult to create unified datasets required for machine learning models. Data quality issues, inconsistent coding standards, and fragmented payer databases further complicate implementation. In addition, healthcare organizations must comply with strict data protection regulations governing patient information, requiring secure data governance frameworks. Integration costs and operational disruptions during system upgrades can discourage smaller healthcare facilities from deploying advanced AI analytics solutions, thereby slowing broader adoption in certain regions.
Rapid expansion of predictive analytics across healthcare systems is opening new opportunities for AI-based revenue cycle insights platforms. Healthcare organizations increasingly rely on predictive models to forecast patient billing patterns, anticipate insurance reimbursement delays, and optimize financial planning. The global healthcare sector generates over 2.3 exabytes of data annually, including billing transactions, patient records, and payer information, creating vast datasets suitable for AI analysis. AI-enabled platforms can evaluate historical billing trends to identify revenue leakage points and forecast reimbursement timelines, enabling healthcare administrators to make proactive financial decisions. Integration with cloud computing platforms is further enabling hospitals to process large datasets efficiently while maintaining secure data storage. Additionally, growing adoption of value-based care models—where reimbursement depends on treatment outcomes rather than service volume—creates demand for advanced analytics capable of tracking cost efficiency and financial performance. These trends present significant growth opportunities for vendors developing scalable AI revenue management platforms.
One of the key challenges affecting the AI Revenue Cycle Insights Platforms Market is the shortage of skilled professionals capable of managing advanced healthcare analytics systems. Implementing AI-driven revenue cycle solutions requires expertise in healthcare data science, medical coding standards, and regulatory compliance frameworks. However, healthcare IT departments frequently struggle to recruit professionals with both clinical and analytics expertise. Workforce studies indicate that nearly 35% of healthcare organizations report shortages of qualified health data analysts, limiting the ability to fully utilize advanced AI platforms. In addition to talent shortages, governance and transparency concerns surrounding AI decision-making are becoming increasingly important. Healthcare providers must ensure that automated billing recommendations remain compliant with insurance regulations and ethical data usage standards. Establishing robust validation frameworks and audit mechanisms for AI algorithms adds operational complexity and implementation costs. These challenges require coordinated efforts between healthcare providers, technology vendors, and regulatory bodies to ensure responsible and effective deployment of AI-driven revenue analytics platforms.
Rapid adoption of predictive denial analytics: Healthcare providers are increasingly implementing predictive analytics engines capable of identifying high-risk claims before submission. Industry surveys show that nearly 62% of large hospitals now use predictive claim validation tools, enabling revenue cycle teams to detect billing anomalies and documentation gaps earlier in the workflow. Hospitals deploying AI-based denial management systems report 35–40% reductions in claim rework tasks, while automated coding validation tools have improved billing accuracy by approximately 30% across multi-specialty hospital networks.
Integration of generative AI for coding automation: Generative AI tools are being integrated into revenue cycle platforms to automate medical coding and documentation review processes. These tools analyze patient records, clinical notes, and billing documentation to recommend accurate coding classifications. Healthcare IT studies indicate that generative AI assistants can automate nearly 45% of routine coding tasks, reducing manual documentation time by 30% and improving coding compliance across hospital billing departments.
Expansion of cloud-based healthcare financial analytics: Cloud computing is transforming revenue cycle management by enabling real-time analytics across distributed healthcare networks. Approximately 58% of healthcare organizations have migrated at least part of their revenue cycle analytics systems to cloud infrastructure, enabling centralized monitoring of billing performance and reimbursement patterns. Cloud-enabled platforms allow hospitals to process millions of claim transactions daily while improving reporting efficiency by nearly 28%.
Growing use of payer-provider data collaboration platforms: AI-powered insights platforms are increasingly facilitating data exchange between healthcare providers and insurance companies. Collaborative analytics systems analyze payer behavior patterns and historical reimbursement data to optimize claim submission strategies. Nearly 47% of integrated healthcare networks are now using shared analytics dashboards with insurance partners, helping reduce payment processing delays by 25% while improving financial transparency across the healthcare ecosystem.
The AI Revenue Cycle Insights Platforms Market is segmented across multiple dimensions including platform type, application area, and end-user industries. These segmentation categories help healthcare organizations select analytics platforms tailored to their operational requirements and financial management strategies. AI-driven revenue cycle insights platforms are widely deployed to analyze claims data, detect billing inefficiencies, and forecast reimbursement patterns. Technology vendors offer specialized solutions ranging from predictive denial management tools to advanced billing analytics dashboards. Adoption patterns vary significantly across healthcare sectors, with hospitals and integrated healthcare networks demonstrating higher implementation rates due to the scale of billing operations and administrative workflows. Application areas include claims management, billing analytics, payment forecasting, and compliance monitoring, while end-users range from hospitals and physician groups to insurance providers and healthcare outsourcing firms. Increasing healthcare data digitization and the growing complexity of reimbursement systems are encouraging broader deployment of AI-driven financial analytics platforms across the healthcare ecosystem.
AI revenue cycle insights platforms can be categorized into Predictive Denial Management Platforms, Billing and Coding Analytics Platforms, Payment Forecasting and Revenue Optimization Platforms, and Compliance & Audit Analytics Platforms. Predictive denial management platforms currently represent the largest segment with approximately 38% adoption, as healthcare organizations prioritize early detection of claim submission errors and insurance policy inconsistencies. These systems analyze historical claim patterns and identify potential rejection risks before submission, significantly reducing administrative rework and billing delays. Billing and coding analytics platforms account for roughly 27% of deployments, as hospitals increasingly automate medical coding validation and documentation review processes. Payment forecasting and revenue optimization platforms are the fastest-growing segment with adoption expanding at nearly 27% annually, driven by healthcare administrators seeking predictive insights for financial planning and reimbursement forecasting. Compliance and audit analytics platforms represent the remaining 35% combined share, providing automated monitoring of regulatory compliance, billing transparency, and payer policy adherence.
• In 2025, a major academic hospital network deployed predictive denial analytics tools capable of analyzing more than 50 million historical claims annually, improving billing accuracy and reducing administrative review workloads across its revenue cycle operations.
Key applications of AI revenue cycle insights platforms include Claims Management, Denial Prediction and Prevention, Billing Accuracy Optimization, Payment Forecasting, and Financial Performance Analytics. Claims management applications currently dominate with approximately 41% adoption, as hospitals require advanced analytics tools to process large claim volumes efficiently while minimizing errors. Denial prediction and prevention applications account for nearly 26% adoption, enabling healthcare providers to proactively identify documentation issues and coding errors before claims are submitted to insurers. Payment forecasting and revenue optimization applications are expanding rapidly and represent the fastest-growing category with adoption increasing at around 28% annually, as healthcare administrators seek predictive insights to improve financial planning and cash flow management. Billing accuracy optimization and compliance analytics applications collectively represent the remaining 33% share, helping healthcare providers maintain regulatory compliance and reduce administrative complexity. In 2025, over 46% of large hospital systems globally reported piloting AI-driven claims analytics solutions, while nearly 38% of healthcare organizations implemented automated coding validation tools to improve billing accuracy.
• In 2024, a national healthcare provider network implemented AI-powered denial prediction software that analyzed more than 12 million claims annually, improving first-pass claim acceptance rates and reducing manual claim corrections across its hospital network.
The AI Revenue Cycle Insights Platforms Market serves a wide range of healthcare stakeholders including Hospitals, Physician Groups and Clinics, Healthcare Payers, and Revenue Cycle Management Service Providers. Hospitals remain the largest end-user segment, representing approximately 52% of total platform adoption, due to their large claim processing volumes and complex reimbursement structures. Multi-hospital networks rely on AI analytics to monitor billing workflows, detect claim anomalies, and forecast financial performance across multiple departments. Physician groups and specialty clinics account for roughly 24% of adoption, as these organizations seek automated solutions to streamline billing operations and reduce administrative workload. Healthcare payer organizations represent the fastest-growing end-user segment with adoption expanding at nearly 29% annually, as insurance companies integrate AI analytics to monitor claim patterns, evaluate provider billing behavior, and optimize reimbursement processing. Revenue cycle management outsourcing providers contribute the remaining 24% share, offering analytics-driven services to healthcare providers seeking outsourced financial operations. In 2025, nearly 44% of large healthcare enterprises reported deploying AI-based revenue analytics systems to optimize financial performance, while over 36% of mid-sized hospitals began testing predictive claim validation tools.
• In 2025, a regional hospital consortium implemented an AI-based revenue cycle analytics platform across 25 hospitals, enabling centralized monitoring of more than 15 million annual claims while improving billing transparency across the healthcare network.
North America accounted for the largest market share at 42.6% in 2025 however, Asia Pacific is expected to register the fastest growth, expanding at a CAGR of 26.8% between 2026 and 2033.
The global distribution of the AI Revenue Cycle Insights Platforms Market reflects varying levels of healthcare digitalization and analytics maturity. North America maintains the largest deployment base due to advanced hospital IT infrastructure, with more than 6,000 healthcare institutions using AI-driven revenue cycle analytics systems. Europe represents approximately 27.3% of global adoption, supported by increasing digital health regulations and cross-border healthcare data exchange initiatives across the EU. Asia-Pacific accounts for about 20.8% of total platform installations, with countries such as China, Japan, and India rapidly expanding healthcare analytics capabilities. South America contributes nearly 5.1% of global deployments, largely concentrated in Brazil and Argentina, where private hospital networks are implementing automated claims processing tools. Meanwhile, the Middle East & Africa region holds around 4.2% market penetration, driven by healthcare digital transformation initiatives in the UAE, Saudi Arabia, and South Africa. Increasing electronic health record adoption—exceeding 70% in developed markets—and rising healthcare transaction volumes, which surpass 10 billion insurance claims annually worldwide, are accelerating regional demand for AI-driven revenue cycle insights platforms.
North America represents approximately 42.6% of global AI revenue cycle insights platform deployments, supported by the region’s highly digitized healthcare infrastructure and extensive use of electronic health record systems. The United States alone processes more than 3.5 billion insurance claims annually, creating strong demand for predictive analytics platforms capable of automating billing verification and reimbursement forecasting. Key industries driving demand include large hospital networks, health insurance companies, and revenue cycle outsourcing providers. Government regulatory frameworks such as the Health Insurance Portability and Accountability Act (HIPAA) and healthcare price transparency rules encourage secure and accurate billing analytics solutions. Technological advancements such as cloud-based claims analytics platforms, AI-driven coding automation, and predictive denial management systems are widely adopted across hospital networks. For instance, Waystar, a regional healthcare payments technology provider, has deployed AI-based claim monitoring tools that analyze millions of healthcare transactions each month to identify billing discrepancies. Regional consumer behavior reflects strong enterprise adoption, with over 60% of major healthcare systems actively investing in AI-driven financial analytics platforms to improve operational efficiency.
Europe accounts for nearly 27.3% of the global AI Revenue Cycle Insights Platforms Market, supported by strong healthcare digitization programs across major economies including Germany, the United Kingdom, and France. Hospitals in these countries increasingly rely on AI-based financial analytics platforms to streamline claims management and comply with complex healthcare reimbursement frameworks. Regulatory initiatives such as the European Health Data Space program and strict data protection regulations encourage healthcare organizations to adopt transparent and explainable AI analytics tools. Approximately 48% of large hospital systems across Western Europe have implemented automated billing analytics platforms capable of processing millions of patient billing records annually. The region is also witnessing rapid adoption of natural language processing-based coding assistants and predictive reimbursement analytics to reduce administrative workloads. A notable regional player, Experian Health, has expanded its analytics solutions across several European healthcare networks, enabling providers to analyze insurance eligibility and billing errors in real time. Consumer behavior trends indicate that regulatory compliance requirements are driving strong demand for explainable AI platforms capable of providing audit-ready financial analytics reports.
Asia-Pacific represents one of the most rapidly expanding markets for AI-driven healthcare financial analytics, accounting for nearly 20.8% of global installations and ranking third in total deployment volume. Major healthcare economies including China, Japan, India, and South Korea are investing heavily in hospital digitization and AI-powered healthcare IT platforms. China alone operates more than 36,000 hospitals, many of which are transitioning toward electronic billing and claims management systems. India’s healthcare IT sector is expanding rapidly, with over 65% of large private hospital networks implementing digital revenue cycle systems. Regional technology hubs in cities such as Tokyo, Shanghai, Bangalore, and Singapore are developing advanced analytics solutions tailored for healthcare administration. A regional technology provider, Wipro, has developed AI-powered healthcare analytics platforms that assist hospitals in monitoring reimbursement performance and insurance claims processing. Consumer behavior variations in this region highlight strong growth driven by mobile healthcare applications and cloud-based analytics platforms, with hospitals seeking scalable AI systems capable of managing large patient billing volumes.
South America accounts for approximately 5.1% of global AI Revenue Cycle Insights Platforms Market adoption, with Brazil and Argentina serving as the primary healthcare technology markets in the region. Brazil alone operates more than 6,800 hospitals and medical centers, many of which are gradually implementing digital billing and claims processing platforms. Healthcare modernization initiatives across public and private hospital networks are encouraging the use of AI-based analytics tools capable of identifying claim errors and monitoring reimbursement cycles. Governments across the region are also promoting digital healthcare infrastructure through technology investment incentives and health system reforms. Private hospital chains increasingly adopt cloud-based revenue cycle analytics platforms to improve financial efficiency and reduce administrative costs. Regional technology provider TOTVS, headquartered in Brazil, has expanded healthcare management solutions that include AI-enabled billing analytics modules for hospitals and clinics. Consumer behavior in South America shows demand tied to healthcare service localization, multilingual billing systems, and integrated hospital information platforms designed to streamline complex insurance reimbursement processes.
The Middle East & Africa region accounts for nearly 4.2% of global AI Revenue Cycle Insights Platforms Market activity, supported by rapid healthcare infrastructure modernization in the United Arab Emirates, Saudi Arabia, and South Africa. Healthcare investment initiatives such as Saudi Vision 2030 and large-scale hospital digitization programs are encouraging adoption of advanced healthcare IT systems capable of automating claims processing and financial analytics. The UAE alone operates more than 180 hospitals and specialized healthcare centers, many of which are implementing digital billing platforms integrated with AI analytics dashboards. Regional healthcare organizations increasingly rely on cloud-based revenue cycle management platforms to monitor insurance reimbursements and reduce claim processing times. Technology partnerships between global healthcare software providers and local hospital networks are accelerating platform deployment. Regional consumer behavior indicates strong demand for integrated digital healthcare management platforms, particularly among private hospital networks seeking to improve operational transparency and financial performance.
United States – 38.2% Market Share: Strong adoption driven by advanced healthcare IT infrastructure, large hospital networks, and high insurance claim processing volumes.
Germany – 9.4% Market Share: Growth supported by widespread hospital digitization initiatives and strict healthcare financial compliance regulations.
The AI Revenue Cycle Insights Platforms Market demonstrates a moderately fragmented competitive environment characterized by a mix of large healthcare IT vendors, analytics technology providers, and specialized revenue cycle management software developers. More than 120 active companies globally provide AI-enabled revenue cycle analytics platforms targeting hospitals, insurance providers, and healthcare outsourcing firms. The market is led by a group of major technology providers that collectively hold approximately 48–52% of the global competitive share, while numerous emerging startups focus on niche capabilities such as predictive denial management, automated coding validation, and reimbursement forecasting analytics.
Competition in the market is primarily driven by continuous product innovation, platform interoperability, and cloud-based analytics capabilities. Vendors are investing heavily in machine learning algorithms capable of analyzing millions of healthcare billing records and insurance claims to provide predictive financial insights. Strategic partnerships between healthcare technology firms and hospital networks are also shaping the competitive landscape, enabling vendors to integrate their platforms directly with electronic health record systems and hospital information systems. Mergers and acquisitions have become increasingly common, particularly as healthcare IT companies seek to expand their AI analytics capabilities. Over the past five years, more than 35 strategic acquisitions have taken place within healthcare revenue cycle analytics technology providers. Vendors are also launching integrated platforms combining AI analytics, robotic process automation, and real-time billing monitoring dashboards to differentiate their offerings. This competitive intensity is expected to drive further innovation and rapid technological advancement across the market.
Optum
Change Healthcare
Experian Health
Waystar
R1 RCM
FinThrive
AKASA
Olive AI
nThrive
CareCloud
Cerner Corporation
Conifer Health Solutions
McKesson Corporation
Cognizant
Wipro
Technological innovation is transforming the AI Revenue Cycle Insights Platforms Market, enabling healthcare organizations to automate complex financial management processes and analyze vast healthcare transaction datasets. Modern platforms integrate machine learning algorithms, natural language processing (NLP), robotic process automation (RPA), and predictive analytics to identify billing anomalies and forecast reimbursement patterns. Healthcare systems generate enormous volumes of administrative data, including billions of insurance claims annually, creating a significant opportunity for AI-driven analytics solutions capable of processing and interpreting this information in real time.
One of the most significant technology trends is the integration of predictive denial management systems that analyze historical claim data to identify billing errors and documentation inconsistencies before claims are submitted. These systems can evaluate millions of historical records and predict high-risk claims with accuracy levels exceeding 85%, significantly reducing claim rejection rates. Natural language processing is also transforming medical coding workflows by automatically analyzing physician notes and clinical documentation to recommend appropriate billing codes. NLP-based coding assistants can automate nearly 40–45% of coding tasks, reducing manual documentation time for healthcare administrators.
Cloud computing technologies are further expanding the capabilities of revenue cycle insights platforms. Cloud-enabled healthcare analytics solutions allow hospitals and multi-location healthcare networks to centralize financial analytics across multiple facilities. These platforms can process tens of millions of billing transactions per day, generating real-time dashboards for administrators monitoring reimbursement performance and insurance payment cycles. Integration with electronic health records and hospital enterprise systems enables seamless data exchange, improving operational visibility across revenue cycle departments.
Emerging technologies such as generative AI assistants and autonomous coding platforms are expected to further enhance platform capabilities. These systems can automatically generate claim documentation summaries, recommend coding adjustments, and provide predictive financial performance insights for healthcare administrators. Combined with advanced data security technologies and blockchain-based audit trails, these innovations are expected to enhance transparency and efficiency across healthcare financial management operations.
• In March 2026, Waystar announced an expanded collaboration with Google Cloud to accelerate its AltitudeAI platform, embedding generative and agentic AI directly into revenue cycle workflows. The platform analyzes data from over one million healthcare providers and billions of payment transactions to automate denial prevention and claims optimization. Source: www.waystar.com
• In July 2025, Waystar signed a definitive agreement to acquire Iodine Software for USD 1.25 billion, integrating clinical intelligence AI with revenue cycle payment software. The combined platform uses large clinical datasets covering over one-third of U.S. inpatient discharges to improve coding accuracy and reimbursement outcomes.
• In August 2025, Oracle Health introduced a next-generation AI-enabled electronic health record (EHR) platform designed for ambulatory healthcare providers in the U.S. The solution uses conversational AI and voice-based workflows to automate documentation and improve administrative efficiency for clinicians and revenue cycle teams.
• In October 2024, Oracle Health launched its Clinical AI Agent, a generative AI system integrated with electronic health records that automatically captures patient interactions, drafts clinical documentation, and extracts coding information to support billing accuracy and compliance across healthcare organizations.
The AI Revenue Cycle Insights Platforms Market Report provides a comprehensive analysis of technologies, applications, and industry sectors shaping the adoption of artificial intelligence within healthcare financial management systems. The report evaluates the integration of advanced analytics platforms designed to optimize billing processes, monitor insurance claim performance, and improve reimbursement forecasting across healthcare organizations. The market scope includes various solution types such as predictive denial management platforms, billing and coding analytics tools, financial forecasting systems, and compliance monitoring solutions designed to support complex healthcare reimbursement environments.
The report covers multiple application areas including claims processing analytics, billing accuracy optimization, denial prediction systems, payment forecasting platforms, and financial performance monitoring dashboards. These applications are widely deployed across hospitals, physician groups, healthcare insurance providers, and outsourced revenue cycle management service providers. Hospitals represent a significant portion of the deployment landscape due to their large transaction volumes and complex reimbursement frameworks, processing millions of claims and billing records annually.
Geographically, the report evaluates adoption trends across North America, Europe, Asia-Pacific, South America, and the Middle East & Africa, highlighting the impact of healthcare digitization initiatives, regulatory frameworks, and hospital infrastructure modernization. The report also explores technology advancements including machine learning, natural language processing, robotic process automation, cloud-based analytics platforms, and generative AI coding assistants that are transforming healthcare financial operations.
In addition, the report examines strategic developments within the competitive ecosystem, including partnerships between healthcare technology providers and hospital networks, increasing venture investment in healthcare AI startups, and the emergence of integrated analytics platforms capable of processing billions of healthcare financial transactions annually. By evaluating technology trends, industry adoption patterns, and operational challenges, the report offers decision-makers a detailed perspective on how AI-driven revenue cycle insights platforms are shaping the future of healthcare financial management.
| Report Attribute / Metric | Details |
|---|---|
| Market Revenue (2025) | USD 2,376.0 Million |
| Market Revenue (2033) | USD 13,418.4 Million |
| CAGR (2026–2033) | 24.16% |
| Base Year | 2025 |
| Forecast Period | 2026–2033 |
| Historic Period | 2021–2025 |
| Segments Covered |
By Type
By Application
By End-User Insights
|
| Key Report Deliverables | Revenue Forecast; Market Trends; Growth Drivers & Restraints; Technology Insights; Segmentation Analysis; Regional Insights; Competitive Landscape; Regulatory & ESG Overview; Recent Developments |
| Regions Covered | North America; Europe; Asia-Pacific; South America; Middle East & Africa |
| Key Players Analyzed | Oracle Health; Optum; Change Healthcare; Experian Health; Waystar; R1 RCM; FinThrive; AKASA; Olive AI; nThrive; CareCloud; Cerner Corporation; Conifer Health Solutions; McKesson Corporation; Cognizant; Wipro |
| Customization & Pricing | Available on Request (10% Customization Free) |
